By Janelle Clausen
Anthony Guerne, now a paramedic in the Greenlawn and East Northport fire departments, carries nearly two decades worth of trauma beneath his smile.
He speaks casually of nearly being stabbed once. He still remembers the face of a man who died in a car accident. It was, and still is, hard for him to calculate how many cardiac arrests and heroin overdoses he’s responded to – how many times he’s barged into the homes of strangers, trying to save their lives, sometimes with their family photos staring at him. His attempts haven’t always been successful. Even when he did everything right, Guerne says, the deaths of patients haunted him.
“I came to the brink a few times,” he said. “I took it personally.”
Guerne, a simulation specialist at Adelphi University in everyday life, says he tried his best to cope with the traumatic incidents of this paid paramedic work in New York City. He drank heavily with his colleagues and walled himself off emotionally from the woman who is now his ex-girlfriend. He became cynical, he says, even as he felt more and more guilt when he failed to save someone. As time went on, he felt alone—even in a culture known for tight-knit camaraderie.
Finally, Guerne decided to seek help. A therapist diagnosed him with post-traumatic stress disorder. This is a mental health issue characterized by intrusive memories, avoiding things that can trigger those bad memories, negative changes in thinking, and more emotional reactions like irritability, overwhelming guilt or shame or self-destructive behavior .
“You would think a lot of people would shy away and leave [the Emergency Medical Services],” Guerne said. But to this day, he continues to take on shifts in addition to his full-time job as a simulation lab specialist at Adelphi University. Simulation labs use mannequins and help nursing students learn medical protocol.
“It’s gotten better,” Guerne said of his symptoms. “Therapy helps.”
Guerne is not alone when it comes to developing mental health issues on the job, but he is nearly in seeking help. According to the Substance Abuse and Mental Health Services Administration, between 10 and 30 percent of EMS practitioners experience PTSD. A recent survey by Fitch & Associates’ Ambulance Service Management program, meanwhile, found that 37 percent of EMS practitioners contemplated suicide and 6.6% actually attempted it. The Centers for Disease Control and Prevention found that only 3.9% of the general population has contemplated suicide while 0.6% attempted it.
Anthony Guerne, now a paramedic in the Greenlawn and East Northport fire departments, carries nearly two decades worth of trauma beneath his smile.
He speaks casually of nearly being stabbed once. He still remembers the face of a man who died in a car accident. It was, and still is, hard for him to calculate how many cardiac arrests and heroin overdoses he’s responded to – how many times he’s barged into the homes of strangers, trying to save their lives, sometimes with their family photos staring at him. His attempts haven’t always been successful. Even when he did everything right, Guerne says, the deaths of patients haunted him.
“I came to the brink a few times,” he said. “I took it personally.”
Guerne, a simulation specialist at Adelphi University in everyday life, says he tried his best to cope with the traumatic incidents of this paid paramedic work in New York City. He drank heavily with his colleagues and walled himself off emotionally from the woman who is now his ex-girlfriend. He became cynical, he says, even as he felt more and more guilt when he failed to save someone. As time went on, he felt alone—even in a culture known for tight-knit camaraderie.
Finally, Guerne decided to seek help. A therapist diagnosed him with post-traumatic stress disorder. This is a mental health issue characterized by intrusive memories, avoiding things that can trigger those bad memories, negative changes in thinking, and more emotional reactions like irritability, overwhelming guilt or shame or self-destructive behavior .
“You would think a lot of people would shy away and leave [the Emergency Medical Services],” Guerne said. But to this day, he continues to take on shifts in addition to his full-time job as a simulation lab specialist at Adelphi University. Simulation labs use mannequins and help nursing students learn medical protocol.
“It’s gotten better,” Guerne said of his symptoms. “Therapy helps.”
Guerne is not alone when it comes to developing mental health issues on the job, but he is nearly in seeking help. According to the Substance Abuse and Mental Health Services Administration, between 10 and 30 percent of EMS practitioners experience PTSD. A recent survey by Fitch & Associates’ Ambulance Service Management program, meanwhile, found that 37 percent of EMS practitioners contemplated suicide and 6.6% actually attempted it. The Centers for Disease Control and Prevention found that only 3.9% of the general population has contemplated suicide while 0.6% attempted it.
Sources: Fitch & Associates' Management Service Management, Centers for Disease Control and Prevention.
But while stress levels are high, a recent mental health survey by the National Association of Emergency Medical Technicians suggests that mental health resources are lacking overall. Only 46 percent of respondents said their EMS agencies provide mental health services, while 37 percent said theirs do not and 15 percent were unsure. Meanwhile, 58 percent of respondents said they were not satisfied with the EMS mental health services provided by their agencies. The most common services provided were the Employee Assistance Program, an employee benefit program that assists workers with personal and work-related problems that hurt their performance, and critical incident stress counseling, which attempts to lessen the impact of a traumatic event.
“If I’m a paid EMT or a paramedic and I need to go out on leave because of a mental health situation, I don’t have the support like I would if I injured my back or injured my leg,” said Richard Stein, an emergency medical technician who has worked in the Huntington and Central Islip Fire Departments, which answer between 5,000 and 6,000 calls per year. “It’s up to the [EMS] provider themselves to seek out that care.”
The Firefighters Behavioral Health Alliance, the only organization in the United States that tracks and validates suicides among firefighters and emergency medical technicians, reported 82 firefighter suicides and 29 EMS suicides this year so far. Jeff Dill, the group’s president, says the actual numbers of suicides are likely higher because most fire departments have not reported numbers to him. Still, this year is on par to match last year’s suicides and already exceeds 2014’s reported total.
“There’s a suicide every 2.7 days, give or take,” Dill said.
Dill noted that suicides in general may also be under-reported because volunteers aren’t necessarily considered firefighters or emergency medical service providers by coroners, since that is not their main profession. Additionally, Dill said his organization also does not have as many contacts in rural areas, meaning the rate of EMS and firefighter suicide might be equal.
“If I’m a paid EMT or a paramedic and I need to go out on leave because of a mental health situation, I don’t have the support like I would if I injured my back or injured my leg,” said Richard Stein, an emergency medical technician who has worked in the Huntington and Central Islip Fire Departments, which answer between 5,000 and 6,000 calls per year. “It’s up to the [EMS] provider themselves to seek out that care.”
The Firefighters Behavioral Health Alliance, the only organization in the United States that tracks and validates suicides among firefighters and emergency medical technicians, reported 82 firefighter suicides and 29 EMS suicides this year so far. Jeff Dill, the group’s president, says the actual numbers of suicides are likely higher because most fire departments have not reported numbers to him. Still, this year is on par to match last year’s suicides and already exceeds 2014’s reported total.
“There’s a suicide every 2.7 days, give or take,” Dill said.
Dill noted that suicides in general may also be under-reported because volunteers aren’t necessarily considered firefighters or emergency medical service providers by coroners, since that is not their main profession. Additionally, Dill said his organization also does not have as many contacts in rural areas, meaning the rate of EMS and firefighter suicide might be equal.
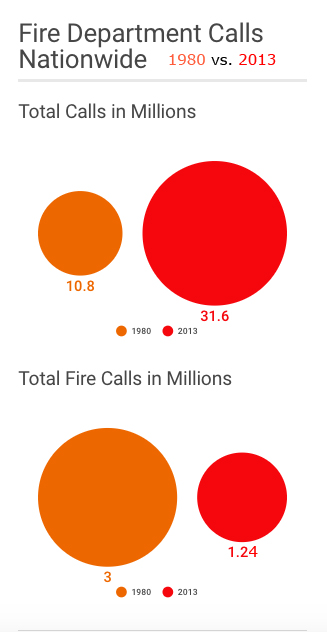 Source: National Fire Protection Association.
Source: National Fire Protection Association.
Compounding the issue is a rising number of medical calls, which increases the chances of being exposed to a traumatic event. The total calls received nationwide roughly tripled to 31 million between 1980 and 2013, according to the National Fire Protection Association. And a much higher percentage of calls are for medical and other emergencies: In 1980, about a third of the nation’s calls to fire and rescue were for fires; today it’s only about 4 percent. Three million of the emergency calls in 1980 were fire; today, only 1.24 million are fire-related The result is individuals fielding more and more medical calls.
“Multiple calls per day is pretty standard,” said Mike Szczygiel , chairman of the National Association of Emergency Medical Technicians’ workforce committee. “They may be exposed to a very terrible event and before they have the opportunity to either mentally or physically recuperate, they’re given another task.”
New York State statistics suggest that most of the people providing basic life support and advanced life support were fire departments. This has led to many departments hiring professional emergency medical professionals to try handling the load of calls better.
“Twenty years ago, the job I have did not exist,” said Eric Zalewski, a full-time teacher and part-time paramedic, referring to his latter position. It was only six or seven years ago that Coram Fire Department mandated that two paramedics be available at all times, he added.
But while there are at least 60,000 people certified in emergency medicine in New York, not all of them are full-time emergency medical service workers, which makes managing the volume of calls even harder.
New York State's Bureau of Emergency Medical Services said it is currently working on their website and will not have updated statistics on medical calls until it's finished. The latest statistics said that in 2007, there were 2.7 million medical calls, and anecdotal evidence from experts suggest these calls are on the rise.
“We’re going to see greater stress on responders,” said Richard Barton, chief executive officer of the International Critical Incident Stress Foundation and a former park ranger, referencing the growing number of medical calls across the country. But because of more people relying upon emergency medical services for treatment, “there’s going to be a greater realization that they need and deserve help,” he said.
“The stress isn’t necessarily the call or the patient. The stress is the resources. It’s not uncommon for us to run four, five six calls at a time,” said Jeremy Bernstein, a volunteer paramedic and dispatcher at Long Beach Fire Department, which fielded nearly 5,000 emergency calls last year. “We [can] run out of ambulances, we run out of personnel, because of the hundred or so volunteers, there’s only 25 or so who are assigned to rescue, and of those 25, not all of them are active all the time.”
The result can be a strained workforce, which makes emergency service workers more vulnerable to mental health issues. Three of the biggest risk factors contributing to the development of mental health issues, Sczcygiel said, include exhaustion from long hours, cynicism stemming from their work, and feeling like they aren’t making a difference.
Interviews with emergency service workers showed that many paid emergency medical technicians and paramedics worked anywhere between 50 and 80 hours a week. In addition, some have to hold a second job to make financial ends meet.
Kyle Castain, who works at the Terryville, Setauket, and Deer Park Fire Departments, as well as Exchange Ambulances of the Islips, a private EMS company, said that sometimes he could be awake for over 48 hours with few naps in between. But Castain described his current week, where he is working 76 hours with two days off, as “easy.” He said that he had to work about 100 hours a week at least once.
“It’s why a lot of people leave EMS… You got to work 80 plus hours a week to make a decent living,” Castain said.
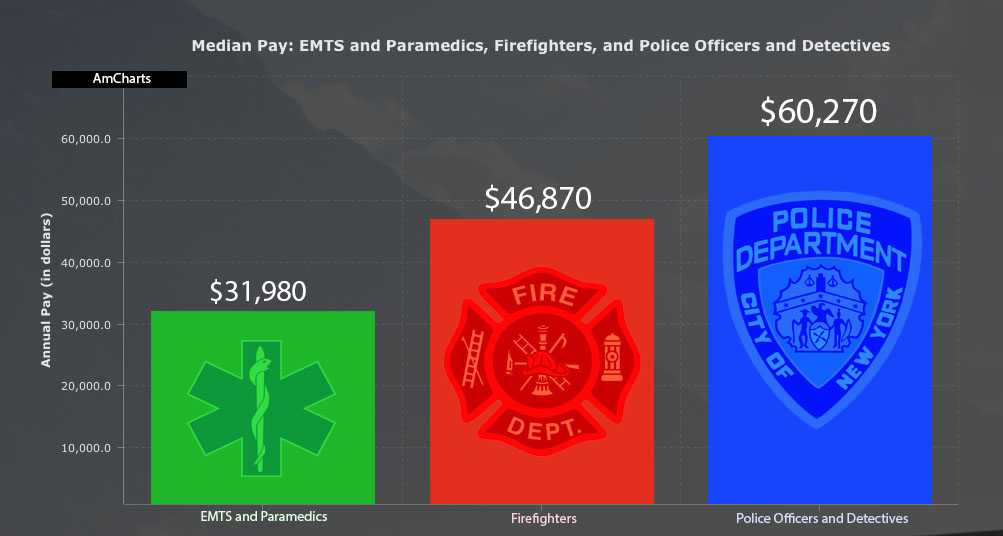
Source: U.S. Bureau of Labor Statistics
“It’s atrocious. Everybody -- and I mean everybody -- has a second job,” said Rob Bruccoleri, an EMT with the New York City Fire Department who also works in Lindenhurst.
Jeff Mitchell, a former firefighter paramedic and psychologist who developed a critical incident stress management model, said that many first responders still fear getting help because of embarrassment and feeling they might be deprived of a promotion or even be fired. While access to mental health help is “gradually gaining ground,” he said that he sometimes feels that there’s barely been progress in the decades he’s worked in the field.
“This is one aspect of this thing we’ve barely made a dent in,” Mitchell remarked. “Years and years of work and it still feels like we’re in 1972.”
Many times a responder will be referred to an employee assistance program, which grants an average six weeks of therapeutical treatment. But, according to Dr. Francine Roberts, a New Jersey-based therapist whose practice specializes in treating responders, many therapists do not have knowledge of the first responder culture.
"It's a hard culture to break into. They're very wary of outsiders," Roberts said, drawing upon her 25 years as a nurse and training with the International Critical Incident Stress Management Foundation and U.S. Department of Veterans Affairs.
Those who are brave enough to seek help, however, also face significant financial hurdles. This is a problem particularly among emergency medical technicians and paramedics, who make significantly less than their firefighter and police counterparts. "It's a mortgage payment," Roberts said. "It's huge."
Jeff Mitchell, a former firefighter paramedic and psychologist who developed a critical incident stress management model, said that many first responders still fear getting help because of embarrassment and feeling they might be deprived of a promotion or even be fired. While access to mental health help is “gradually gaining ground,” he said that he sometimes feels that there’s barely been progress in the decades he’s worked in the field.
“This is one aspect of this thing we’ve barely made a dent in,” Mitchell remarked. “Years and years of work and it still feels like we’re in 1972.”
Many times a responder will be referred to an employee assistance program, which grants an average six weeks of therapeutical treatment. But, according to Dr. Francine Roberts, a New Jersey-based therapist whose practice specializes in treating responders, many therapists do not have knowledge of the first responder culture.
"It's a hard culture to break into. They're very wary of outsiders," Roberts said, drawing upon her 25 years as a nurse and training with the International Critical Incident Stress Management Foundation and U.S. Department of Veterans Affairs.
Those who are brave enough to seek help, however, also face significant financial hurdles. This is a problem particularly among emergency medical technicians and paramedics, who make significantly less than their firefighter and police counterparts. "It's a mortgage payment," Roberts said. "It's huge."
|
One organization that has tried to fill the void is On-Site Academy in northern Massachusetts. Founded by Hayden Duggan, a psychologist and firefighter whose colleagues came to him for help, and his wife Valerie, the clinic evolved over 25 years from a “five-day boot camp” into a non-profit residential training center for critical incident stress management.
The program focuses on first responders, including emergency medical service workers. It also treats military personnel and veterans. |
Executive Director Valerie Duggan, a clinically trained social worker, said that On-Site Academy sees between 200 and 300 people a year. The center offers yoga, eye movement de-sensitization and reprocessing (EMDR), a psychotherapeutic technique that aims to lessen the emotions felt when remembering a traumatic event, peer support and de-briefing, to help first responders organize their thoughts and address them. They also have an anger management and substance abuse program.
“They really get to deal with the underbelly of human life,” Duggan said. “The body wasn’t meant to do that over and over, day after day. They give a huge chunk of their souls and a huge chunk of their lives to help us.”
“They really get to deal with the underbelly of human life,” Duggan said. “The body wasn’t meant to do that over and over, day after day. They give a huge chunk of their souls and a huge chunk of their lives to help us.”
While this doesn’t always culminate in full-blown PTSD and suicide is still relatively rare, Jeff Dill said that virtually every person in the fire service or EMS experiences at least one symptom of job-related stress. They are particularly vulnerable to flashbacks and sensitivity to memories being triggered.
“We take that home,” Dill said, referring to what first responders encounter. “I don’t care what anyone says.”
Still, many said that working within a fire department’s emergency medical services can be both rewarding and stressful.
Nick Viscusi ,who has worked in the emergency medical services since 2010, described calls he’s answered as “war stories.” One of them was the death of a landscaper who was hit by a woman who was driving while impaired by drugs.
“He didn’t see it coming, thankfully,” Viscusi said. “We think he just got shit whipped and snapped his neck and was killed before he hit the ground.”
Viscusi said he manages to cope with the stress of the job by separating it from his home life.
“Do I care about people? Absolutely. Do I take my work home with me? I try my best not to,” Viscusi said. “What happens at work stays at work. I don’t need anything of what I’ve seen or done to follow me into my personal life.”
Anthony Guerne, meanwhile, finds that many people still doubt that mental health issues exist. He gets into arguments about post-traumatic stress disorder with the very same man who inspired him to join the emergency medical services.
“He believes it’s just a crock and still to this day,” Guerne said. “There’s a lot of holdouts. You don’t want to seem less of a person, less of what you are.”
But Guerne still makes it a point to bring up post-traumatic stress disorder and its dangers whenever he can, frequently giving presentations and mentioning it to students when the opportunity arises.
“It needs to be out there in the forefront and that it’s not a problem if somebody wants to ask for help,” Guerne said. “You’re not alone. The ‘alone’ is what made me come to the brink.”
“We take that home,” Dill said, referring to what first responders encounter. “I don’t care what anyone says.”
Still, many said that working within a fire department’s emergency medical services can be both rewarding and stressful.
Nick Viscusi ,who has worked in the emergency medical services since 2010, described calls he’s answered as “war stories.” One of them was the death of a landscaper who was hit by a woman who was driving while impaired by drugs.
“He didn’t see it coming, thankfully,” Viscusi said. “We think he just got shit whipped and snapped his neck and was killed before he hit the ground.”
Viscusi said he manages to cope with the stress of the job by separating it from his home life.
“Do I care about people? Absolutely. Do I take my work home with me? I try my best not to,” Viscusi said. “What happens at work stays at work. I don’t need anything of what I’ve seen or done to follow me into my personal life.”
Anthony Guerne, meanwhile, finds that many people still doubt that mental health issues exist. He gets into arguments about post-traumatic stress disorder with the very same man who inspired him to join the emergency medical services.
“He believes it’s just a crock and still to this day,” Guerne said. “There’s a lot of holdouts. You don’t want to seem less of a person, less of what you are.”
But Guerne still makes it a point to bring up post-traumatic stress disorder and its dangers whenever he can, frequently giving presentations and mentioning it to students when the opportunity arises.
“It needs to be out there in the forefront and that it’s not a problem if somebody wants to ask for help,” Guerne said. “You’re not alone. The ‘alone’ is what made me come to the brink.”